Whether you’re new to hiking, you’ve been away from the trail for a while, or even if you’re a regular hiker thinking of taking on more challenging trails, you may wonder if you’re physically ready. No matter how badly you want to get outdoors and hike, a lack of confidence in your own physical condition can be hard to overcome.
The best way to deal with that fear is to take positive action! If you’re not sure you’re ready, you can take steps that will help to prepare you and boost your confidence, all while building your overall physical fitness – not just for hiking, but for all aspects of life. A fitter, healthier you will be ready for more hikes and a better quality of life!
Maintaining a healthy diet and incorporating a balanced exercise routine into your life are great ways to get ready to hike, but that doesn’t mean you can’t hike until you’re fit.
Hiking can be both a fitness goal on its own and an important step toward reaching your ideal level of fitness. Regular walks can be an important part of your fitness routine. One of the best ways to get fit (for hiking or any other physical activity) is to hike, at whatever level you’re ready to take on! If that means short hikes, that’s fine. Every step down the trail is a step in the right direction.
Your Off-Trail Diet
Diet is a central part of any fitness program at any age, and it takes on particular importance as we age. A healthy, well-balanced diet can work wonders on our preparations for hiking. Eating right can help us drop excess weight, gain muscle, and get the vitamins and nutrients we need to keep us fit to hike.
Writing about diet can be a minefield. There are dozens of specialized diets out there and many of them have a passionate following. You can get a balanced, nutritious diet from most diets, though in some cases you may need to select foods carefully or use supplements to get all of the nutrients you need.
We’re not going to try to compare or recommend specialized diets or referee the debates between gluten-free vegans and keto believers. Those are individual choices and we respect all of them! We will take a look at some diet issues that are specific to older people and some features that are common to most health-conscious diets.
Diet And Ageing: Special Concerns
There are many different ways of eating and innumerable diet plans. However we choose to eat, we all have to face certain realities as we age. Our bodies change and our nutritional needs change with them. Let’s look at a few specific areas of concern for all older people.
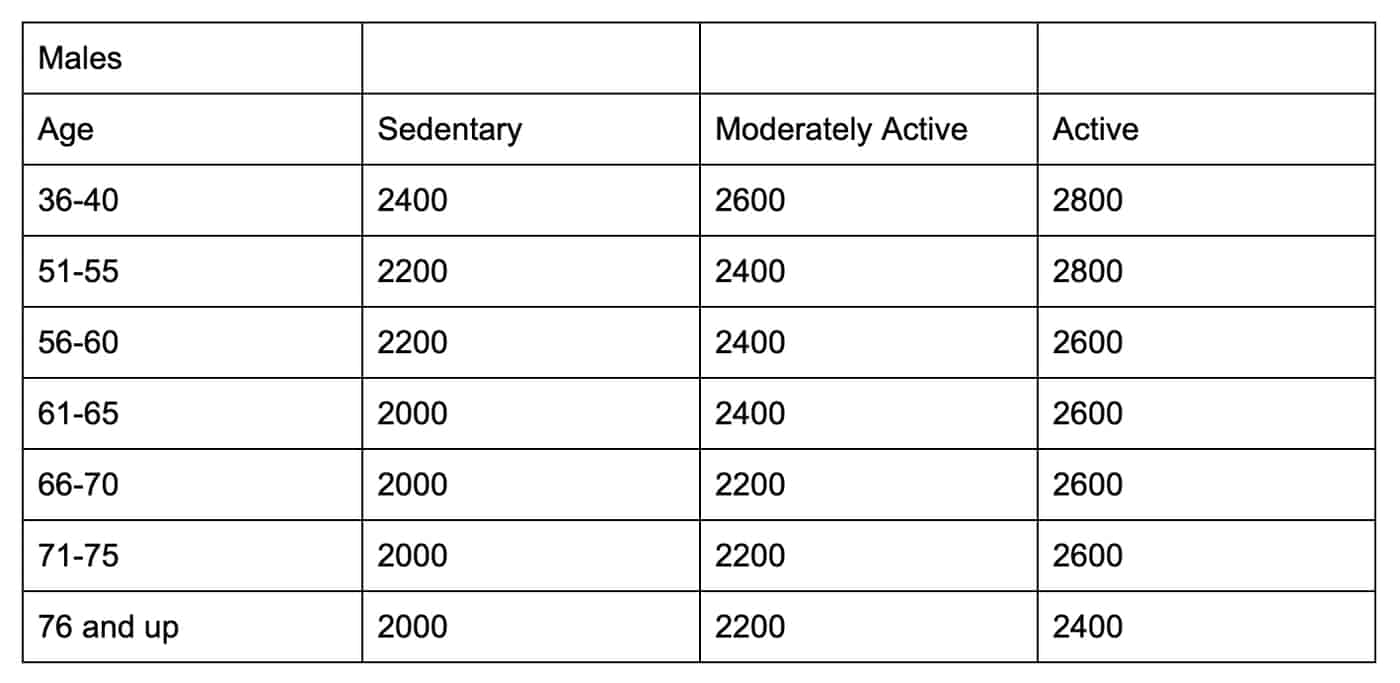
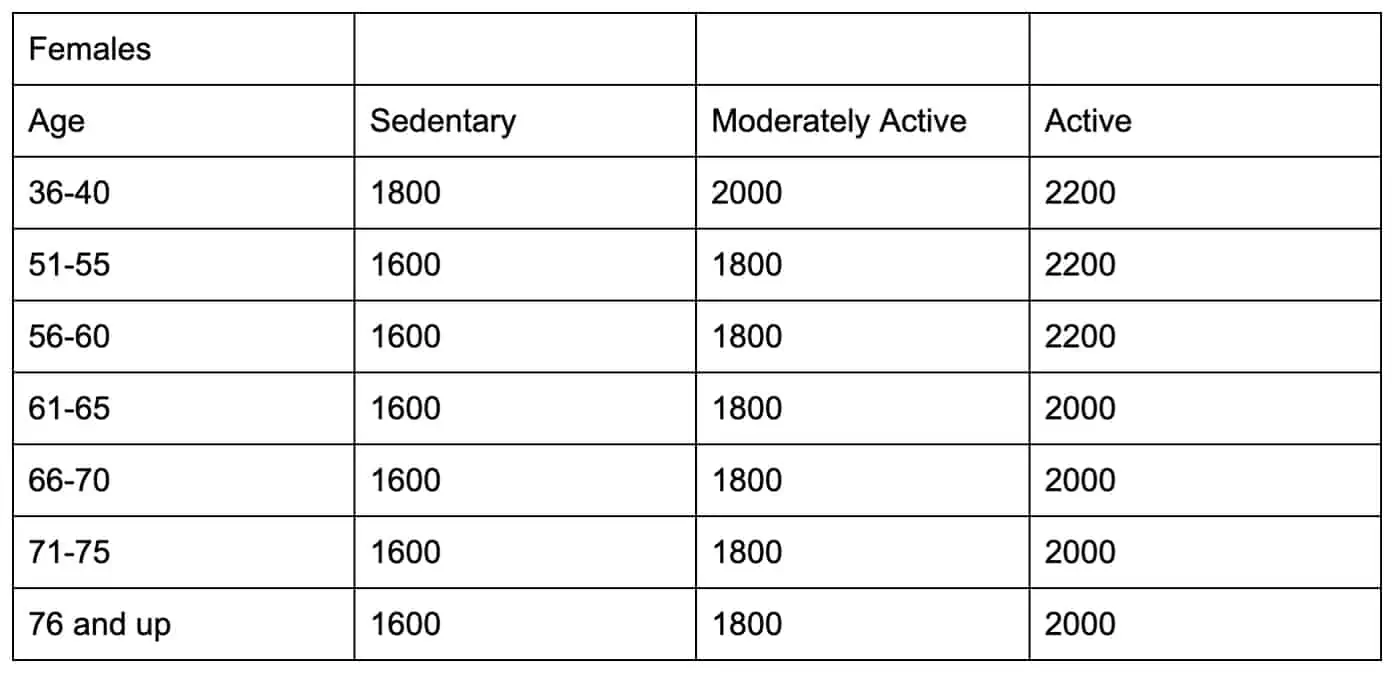
We need fewer calories. Our metabolism slows as we age, meaning our bodies require less energy to function as we get older. We can offset that to some extent with activity and exercise, but we’ll still need fewer calories than a younger person of a similar activity level would. The reduction in caloric needs is more dramatic for men than for women and can vary among individuals. These are average figures from the US Dept of Health:
“Moderately Active” means a level of activity “equivalent to walking about 1.5 to 3 miles per day at 3 to 4 miles per hour, in addition to the activities of independent living”.
“Active” indicates a level of activity “equivalent to walking more than 3 miles per day at 3 to 4 miles per hour, in addition to the activities of independent living”. Source.
Lower calorie requirements can create problems. The first is one many of us know all too well: if we keep eating the same way as we age, we’re likely to find ourselves gaining weight. The same diet that kept us in a caloric balance when we were 40 can easily have us taking in more energy than we burn – and storing fat as a result – at 60.
The second potential problem is less obvious but may have an even greater impact. We need fewer calories as we age, but there are several critical nutrients that we actually need more of the older we get.
If we meet that lower demand for calories by cutting back on the amount we eat, we may not get enough of those essential nutrients. In many older people, that problem is complicated by the use of maintenance medications and reduced levels of stomach acids, both of which can make some nutrients difficult to metabolize. Even if we’re eating enough food, we still may not be getting enough nutrients!
If we’re cutting down on the amount we eat, whether it’s because we want to lose weight or because we just aren’t that hungry anymore, we have to be conscious of where we cut and what we might have to add in to make sure we’re getting the nutrients we need.
Here are a few areas of particular concern:
Protein is a vital part of the muscle-building process. To boost your protein intake as you reduce calories, you may have to add more protein-rich foods to your diet and emphasize foods that give you protein without the calorie-dense fat. Good examples of high-protein, low fat foods include: fish, poultry, lean meats, and legumes. A protein-rich diet combined with regular strength training can help you offset the natural muscle loss that occurs with age!
Calcium is a vital nutrient for bone growth and calcium deficiencies are closely linked to osteoporosis. Many older Americans don’t get enough calcium and evidence suggests that this deficiency is a factor in decreasing bone mass. You can boost your calcium intake with dairy products like milk, cheese, and yogurt, as well as dark green vegetables like broccoli and kale. Sesame seeds are also extremely rich in calcium and other micronutrients.
Vitamin D promotes calcium absorption and helps the body maintain its calcium level. Even if your diet contains enough calcium, you may not be able to use it if you don’t get enough vitamin D. Your body synthesizes vitamin D when you expose yourself to the sun, but many older Americans have limited sun exposure and some sources state that approximately 90% of those between 50 and 70 do not get enough vitamin D. Fatty fish like salmon, mackerel, and tuna are great sources of vitamin D, as are beef liver and cheese. Vegetarians or those who don’t care for fish may need to take vitamin D supplements, especially if their sun exposure is limited.
Fiber helps move food through the digestive process and promotes healthy digestion. It is also believed to be a significant factor in preventing diverticular disease. Many Americans who depend heavily on processed foods don’t get enough fiber. Beans, legumes, many vegetables, whole grains, nuts and seeds, and many fruits, notably apples, bananas, and pears, are good sources of fiber. Whole grains are an important source of fiber and individuals who choose diets that limit or eliminate carbohydrates may have a hard time getting enough fiber. If you’re on one of these diets, you may need to consider fiber supplements.
Vitamin B12 is required for forming red blood cells, maintaining brain functions, and other critical physical processes. It is naturally found in animal-based foods like fish, shellfish, meat, poultry, eggs, and dairy products. Dietary vitamin B12 is released by the action of stomach acids. A significant number of older Americans have atrophic gastritis, which limits acid secretion and blocks the absorption of dietary vitamin B12. Individuals with atrophic gastritis and those who prefer to minimize or completely avoid consumption of animal-sourced foods may need vitamin B12 supplements.
Folate or Folic Acid is another B vitamin that works with vitamin B12 to protect cognitive functions in older people, including response speed, sustained attention, and visual-spatial skills. You can build folate into your diet with meat, fish, poultry, beans, green leafy vegetables, and many fruits.
Potassium is essential for bone growth and cell function. Studies have indicated that it also helps you excrete excess sodium, which plays a role in controlling high blood pressure. Many fresh fruits and vegetables, notably bananas, avocadoes, sweet potatoes, and green leafy vegetables are rich in potassium, and if your diet emphasizes these foods, you probably won’t need any additional potassium. If you do choose to use potassium supplements, be careful: too much potassium can be dangerous, especially for people with kidney problems.
Magnesium is involved in numerous physiological processes and magnesium deficiencies are linked to a wide range of health problems, including cardiovascular disease, hypertension, and diabetes. According to The Journal of Nutrition, older people often don’t get enough of this vital nutrient. Like potassium, magnesium is found in many fresh fruits and vegetables, and a diet that includes these foods on a daily basis will usually provide enough magnesium to meet your needs. Individuals who don’t often eat fresh fruits and vegetables may need supplements.
Omega-3 Fatty Acids have the potential to reduce both cognitive decline and cardiovascular events in older adults. While the benefits of these nutrients are still being studied, many experts advise regular Omega-3 Fatty Acid intake, either by eating regular portions of fish like salmon or herring or from some other foods, like walnuts and flax seeds. Omega-3 supplements are also available.
All of these nutrients are available from dietary sources, and most experts agree that the best way to meet your nutrient needs is through a balanced diet. People with different diet preferences may have to manage that balance in different ways. A diverse menu emphasizing fresh, locally produced food that includes plenty of fresh vegetables and fruits will meet most dietary requirements for most people.
To keep our nutrients up even as we reduce the amount we eat, older people need to emphasize nutrient-dense foods that pack a lot of value into a limited portion with a relatively low calorie count.
That’s not always easy to do, especially for people whose diets or preferences exclude common food groups or those who don’t always have access to fresh whole foods. If our diet falls short in some areas, we still have options in the form of supplements.
Supplements For Daily Use
Like diet, supplements can be a complicated topic. Some people swear by them, others think they’re unnecessary and prefer to get their nutrients exclusively from food. Advertisements make dramatic claims, but the fine print always contains the words “no approved therapeutic claims”. Some doctors recommend supplements for patients who may not be getting enough of certain nutrients in their diets. Some experts also worry that older Americans are overusing supplements.
How do we cut through these sometimes contradictory claims and decide which supplements we really need?
Let’s start with the basics. Our bodies need minimum amounts of certain substances. In most cases, enough is just right: taking in more than we need rarely helps and can sometimes do actual harm.
Ideally, we’d get all we need from our food, but for a variety of reasons, we sometimes don’t. When we don’t, we can turn to supplements to make up the shortfall.
There are several reasons why we might need supplements to get enough of some key nutrients:
Digestive problems could make it difficult to metabolize some nutrients. For example, people who suffer from atrophic gastritis may need to take vitamin B12 supplements.
Diet choices may make some nutrients difficult to obtain. For example, vegetarians or vegans might need to take supplements to boost their intake of vitamin B12 and vitamin D; people on low-carb diets may wish to take added fiber; and people who don’t like eating fish might choose to take Omega-3 fatty acid supplements.
Individual medical requirements might indicate a need for more of some nutrients than some individuals can reasonably expect to get from food. Individuals at risk for osteoporosis, for example, might need calcium and vitamin D supplements.
Seasonal or regional lack of access to some fresh foods might make it difficult to get full nutrition from dietary sources at some times. Supplements can help to fill the gap.
Prescription drug side effects may interfere with the absorption of some nutrients. Drug-nutrient interactions may affect the body’s ability to use a wide variety of nutrients and may make supplements necessary.
In any of these cases, a well-chosen supplement can fill the gap between what your diet can provide and what your body needs.
Supplements have their place and can play a vital role in bridging gaps between what diet provides and what our bodies need. That doesn’t mean they are always helpful. Some may not be helpful and some may be harmful, and they can also be quite expensive.
In some cases, the evidence on a supplement simply isn’t clear. Many people who suffer from arthritis and other joint disorders use supplements containing glucosamine, chondroitin, or a combination of the two. Many swear that these supplements help their joint problems. Medical studies have been unable to verify these claims.
The choice to use a supplement is your decision, but it’s always wise to do thorough research into a supplement and seek professional advice if you aren’t sure. Most have not been thoroughly tested for either safety or efficacy. Some supplement ingredients can even be dangerous.
You may wish to discuss your diet and physical needs with a doctor or nutrition specialist before using supplements. Always tell your doctor what supplements you’re using: some supplements may interact with prescription drugs.
If you do choose to use supplements, always select reputable brands. Look for seals that indicate that a product has been independently tested. Studies have found that many supplements do not contain the advertised ingredients and many are tainted with contaminants.
Diet is a critical part of building up our fitness and preparing our bodies for longer and more challenging hikes, but it’s not the only part. Let’s look at the other component of physical preparation: exercise.
READ MORE
For more, check out these popular buyer's guides:
5